ORAL SURGERY
1. Information on the PRF (Platelet Rich Fibrin) protocol
Surgeon, anaesthesiologist and pain specialist Dr Joseph Choukroun devised the PRF method in 2001. The PRF method is a cutting-edge means for promoting wound healing, exerting its effect through white blood cells, growth factors and cytokines present in the blood. In the PRF protocol blood is drawn from the patients and centrifuged at a low speed (PRF centrifuge). The natural coagulation process forms a fibrin coagulate abundant in growth factors and white blood cells (leukocytes) which serve an extracellular matrix function. The extracellular matrix promotes the formation of new blood vessels and the new vascular network, keeping the wound moist and slowly but continuously releasing growth factors, cytokines, etc. required for healing.
In the course of research Dr Chokroun and his team also developed protocols A-PRF (Advanced PRF) and I-PRF (Injectable PRF). A thick sheet-like membrane can be prepared from A-PRF (a protective membrane of gel-like consistency) with which to “dress” the wound. I-PRF is a fibrin of a thinner consistency that can be pumped into a syringe with which to irrigate the surgical area or bone. A great number of mesenchymal stem cells are present in I-PRF
The two protocols may even be combined with more substantial amounts of blood drawn (when preparing to perform a bone graft of a larger scale, e.g. sinus lift), where A-PRF is used as a membrane or matrix protecting the wound, whereas I-PRF is mixed with the bone graft material. The mixture of the fibrin clot derived and bone graft material will result in an easy-to-handle sticky bone consistency perfectly suited for administration and gluing onto the bone graft area, facilitating the surgeon’s job.
Advantages of using PRF:
- Pain relieving effect, with pain resolving in as little as one day.
- Administration of post-surgery antibiotics is not required since the fibrin clot abundant in white blood cells decrease the risk of infection.
- The fibrin clot keeps the wound moist and promotes the formation of blood vessels (angiogenesis), which is conducive both to wound healing and bone formation.
- The procedure may also be applied on patients on anticoagulant medication but fibrin clot formation takes a few minutes longer.
- Indications for the PRF protocol.
- oral surgeries such as tooth extraction, tooth implantation, sinus lift, bone graft, resection.
- periodontal treatments such as pocket cleaning, open or closed curettage, removal of connective tissue grafts, soft tissue surgeries, tunnel technique.
Further Informations
2. Tooth extraction
Tooth extraction is required when the tooth can no longer be preserved with conservative techniques (root treatment, tooth filling, gum disease) as the extent of the damage or periodontitis is too large for the tooth to be suitable for a crown attachment or filling. Removal of these teeth can be effected simply with a dental plier as a routine tooth extraction or as part of a surgery in which the tooth and tooth root are removed following surgical exposure and the gum is sealed with sutures thereafter.
Surgical tooth extraction is mainly indicated with rear molars, erupted wisdom teeth and tooth broken under the gum (e.g. the chipping of a crown of a tooth having undergone root canal treatment due to an accident). In such instances the multi-rooted teeth are dissected, that is, the roots are separated and then removed one by one.
The removal of non-erupted (impacted) wisdom teeth embedded in the jawbone, sinus and the palate call for a major oral surgery. In the vast majority of cases taking antibiotics and painkillers is part of the treatment.
Further Informations
3. Resection
If the root canal treatment fails on repeated occasions, the endodontic needle breaks under the root canal, the root is highly curved or the root canal treatment turns out less than 100% successful, chronic inflammations and pus pockets or cysts develop on the infected root tip. When performing resection a flap is cut open from the gum at the infected root, a hole is bored sideways into the jawbone and the infected root tip, or apex, is cut off and scraped (apicoectomy). In other words, resection means both the removal of the infected root tip and the cleaning of the adjacent area. By this intervention, a tooth slated for extraction is given one more chance with a good likelihood of being rescued. Treatment is always performed in local anaesthesia or conscious sedation. Complete healing time is 6 to 12 months. Follow-up X-rays are due every half a year and 2 or 3 years are required to establish whether the intervention was successful.
Further Informations
4. Sinus Lift
In some cases, the posterior upper jaw (maxilla) loses significant bone volume due to inflammation, infection, or periodontal disease. After tooth loss, only 3–5 mm of bone height may remain, whereas the shortest available dental implants start at 7 mm in length. To enable implant placement, bone augmentation is required to increase the height of the jawbone.
A sinus lift is a surgical procedure in which bone graft material is placed into the patient’s maxillary sinus, between the jawbone and the sinus membrane, typically in the area of the molars. This procedure is also known as sinus augmentation. By elevating the floor of the sinus—hence the term “lift”—we create the necessary vertical space. The graft material stimulates the formation of new bone, increasing both the height and width of the jawbone, thus allowing for the placement of implants longer than 7 mm.
The procedure can also be performed under conscious sedation, if requested.
Further Informations
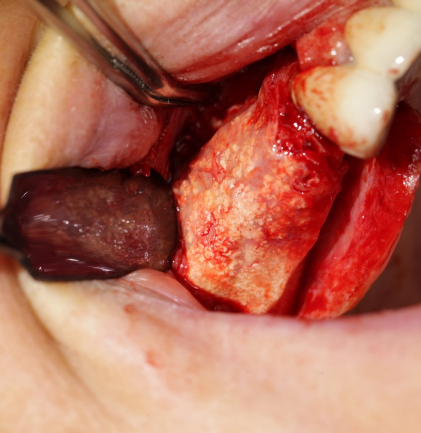
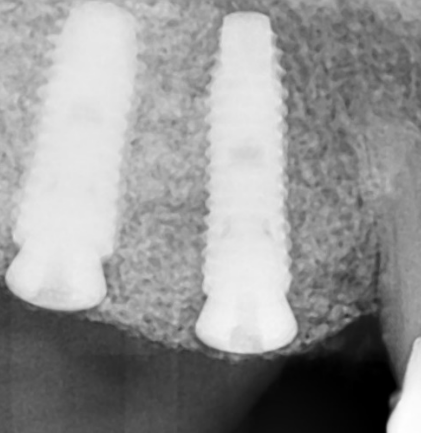
5. Horizontal and vertical ridge augmentation (Urban technique)
Horizontal and vertical ridge augmentation is a complicated surgery both for the patient and the staff performing it. Bone augmentation is essentially guided bone formation and regeneration (GBR, Guided bone regeneration, for short) with a view to providing sufficient bone mass for the mounting of implants. As compared to conventional bone graft procedures (sinus lift) such surgeries are capable of creating incomparably greater bone mass in the jawbone.
In the course of bone augmentation, a mixture of autogenous bone and bone graft material is used. Autogenous bone is derived from the lower jawbone (mandible) and ground using a bone mill. The bone-grafted area is covered with a membrane (Cytoplast, Lyoplant) and secured by means of titanium pins (Master Pin Meisinger). The surgical areas are sealed with non-resorbable sutures for strong retention. Non-resorbable sutures are way less prone to the adhesion of plaque reducing thereby the risk of infection.
Foreign patients are required to plan for a stay of at least 10 days, so we can carry out daily monitoring and remove the non-resorbable sutures. Following horizontal and vertical bone augmentation the patient is required to rest for at least 1 week.
Further Informations
6. bone substitutes
Horizontal and vertical ridge augmentation is a complicated surgery both for the patient and the staff performing it. Bone augmentation is essentially guided bone formation and regeneration (GBR, Guided bone regeneration, for short) with a view to providing sufficient bone mass for the mounting of implants. As compared to conventional bone graft procedures (sinus lift) such surgeries are capable of creating incomparably greater bone mass in the jawbone. In the course of bone augmentation, a mixture of autogenous bone and bone graft material is used. Autogenous bone is derived from the lower jawbone (mandible) and ground using a bone mill. The bone-grafted area is covered with a membrane (Cytoplast, Lyoplant) and secured by means of titanium pins (Master Pin Meisinger). The surgical areas are sealed with non-resorbable sutures for strong retention. Non-resorbable sutures are way less prone to the adhesion of plaque reducing thereby the risk of infection. Foreign patients are required to plan for a stay of at least 10 days, so we can carry out daily monitoring and remove the non-resorbable sutures. Following horizontal and vertical bone augmentation the patient is required to rest for at least 1 week.
As a result of tooth extraction and certain infections the quantity and quality of the bone may substantially deteriorate. Implantation at areas having undergone significant bone loss calls for a procedure called bone-graft in which both the width and height of the bone is increased. Following bone-graft a 6 to 9 month healing period ensues. During this time, the mixture of the body’s own bone material and the inserted bone graft material transforms into new bone making the bone suitable for implantation.
Further Informations
7. Membrane
When performing a bone graft the dentist attaches a mixture of native bone and bone graft material to the new bone. In order to be able to control the area where the newly formed bone develops, we secure the bone graft material by means of membranes (GBR = guided bone regeneration). This process can be conceived of as attaching a new wall to an old and thinner wall but in order to adequately cement them together shuttering is required. The same applies to bone grafting. It does not merely suffice to add the new bone, the new bone also needs to be secured to the old wall, in other words, the two walls should be firmly held together for the duration of healing. A variety of membranes are available for this purpose. Resorbable membranes (Jason, Lyoplant) gradually resorb under the gum following surgery, and therefore call for no second surgery to remove them.
Non-resorbable membranes (Cytoplast, Permamem) are applied where the extent of bone loss indicates the riveting of a titanium-reinforced membrane to the bone in order to hold the newly inserted bone grains in position for the duration of healing. The area needs to be surgically exposed to remove the membrane after 6 to 9 months’ healing, which allows for unhindered implantation into the newly formed bone. At our clinic, we chiefly use:
Further Informations
8. Sutures
From the point of view of healing, the kind of seam used at the different interventions is crucial. Following a bone grafting procedure, tension-free seams are required that can hold the gum together. Here we make mention of two types of sutures: resorbable sutures slowly absorb after surgery, growing thin in a few days and giving way slowly before being ejected. The other type of suture is a non-resorbable, thin and very durable monofilament, teflon (PTFE). It is removed in a scheduled fashion rather than being allowed to come off on its own accord.